Food as Medicine: How a Hospital Kitchen Is Transforming Cancer Care for Children in Uganda
WHO and IIPAN
23 Mar 2026
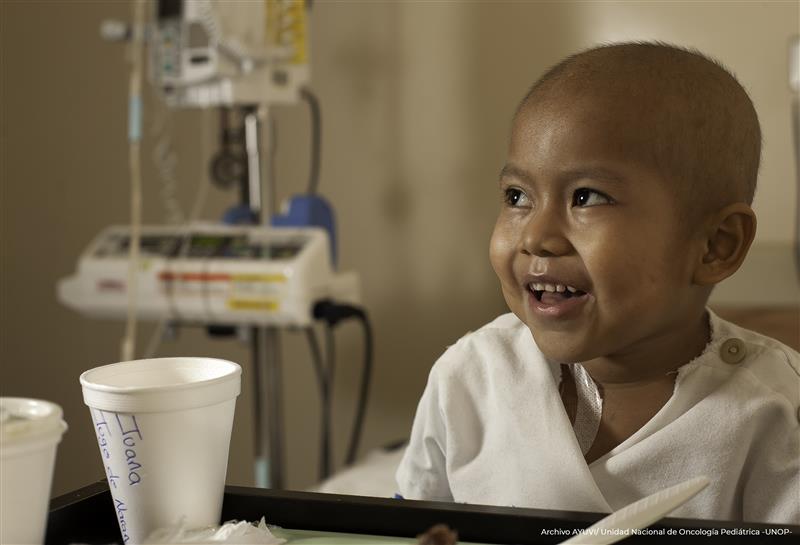
The Global Nutrition Challenge
Malnutrition affects up to 88% of children with cancer in Africa,1 contributing to higher mortality, increased infections, treatment-related complications, and poorer quality of life.2,3 Nutritional care plays a critical role in improving both survival and treatment outcomes for children with cancer. Evidence shows that proactive nutrition care can improve survival by up to 30%4 and reduce several treatment-related toxicities.5–7
Many hospitals in low- and middle-income countries are unable to meet the nutritional needs of children with cancer. Standard hospital meals often fail to meet daily calorie and protein requirements, and therapeutic foods are either prohibitively expensive or inconsistently available.8 This is not an isolated occurrence; a review of integrated nutrition programs within health systems identified the limited availability of nutrition products as a common barrier to effective implementation.9
To address these constraints, clinicians have long relied on locally enriched family foods for nutritional rehabilitation.10Building on this tradition, the International Initiative for Pediatrics and Nutrition (IIPAN), a clinical nutrition capacity-building program based at Columbia University Irving Medical Center, has developed its Food as Medicine programs for implementation across all IIPAN sites. These programs establish hospital kitchens, train staff, and develop recipes to provide homemade therapeutic foods and formulas using affordable, locally available ingredients.
The Innovation
Uganda Cancer Institute (UCI), located in Kampala, is Uganda’s leading public cancer care facility and sees an average of 90 children with cancer each day. Since 2021, IIPAN has partnered with UCI to establish a dedicated nutrition program for children with cancer.
At the heart of this program is Joseph Semujju, a registered nurse by training, who now serves as the full-time pediatric oncology nutritionist. Early in the program, Joseph and the IIPAN team observed that many children were unable to meet their nutritional needs through standard hospital meals or the available supplies of commercial therapeutic foods and formulas.
In response, UCI, IIPAN, and local donors renovated a space within the pediatric oncology ward to create a fully functioning Food as Medicine kitchen directly on the ward. Equipped with a stove, refrigerator, freezer, sink, and essential kitchen tools, this kitchen became the foundation of the hospital-based Food as Medicine program.
The IIPAN team focused on developing nutrient- and calorie-dense foods catered to the local setting. After testing several recipes for nutritional value, cost, and patient acceptability, the kitchen now regularly produces a protein-dense paste and a coconut-based smoothie for children who are acutely malnourished or struggling to meet their calorie and protein needs. In addition, all patients receive daily nutrient-dense porridge, eggs, and bananas.
Coconut-based smoothie recipe | ||
Coconut meat | 485 g | Servings: 20 servings, total volume 2000 mL (1 serving = 100 mL) Tools needed: blender, spoon, liquid measuring cup, measuring spoon, plate, serving cups, kitchen weigh scale Procedure: 1. Wash hands with soap and clean water for 20 seconds before preparing food. 2. Ensure the tools and preparation surfaces have been cleaned. 3. Place small plate on weigh scale and zero out scale. Using a spoon add coconut meat onto plate to appropriate weight and add to blender. 4. Measure all liquid ingredients with liquid measuring cup or spoon to required volumes and add to a blender. 5. Add bananas to blender. Pulse for about 30 seconds. 6.Once reaching a smooth consistency, pour into a liquid measuring container to the desired volume for patient. Once appropriate volume assessed, pour into a serving cup. 7. Store remaining formula in a sealed container in the refrigerator. |
Vanilla extract | 6 mL | |
Yellow banana | 1 1/3 medium | |
Water | 300 mL | |
Multivitamin syrup | 5 mL / child | |
Nutrient information: Per 100 mL serving: 94 calories, 1 g protein, 5 g carbohydrates, 2 g fiber, 8 g fat | ||
This effort is supported through a shared partnership model: UCI contributes part-time staff to prepare the therapeutic foods, a local foundation generously funds the monthly cost of ingredients, and IIPAN works together to create tasteful and healthy recipes to support children and their families during this difficult time. Together, these efforts ensure that every child undergoing cancer treatment receives nourishing, therapeutic foods.
The Impact
Every day, the Food as Medicine program at UCI provides nutritious, therapeutic foods and formulas to approximately 90 children undergoing cancer treatment. Among children with severe acute malnutrition, 99.3% are now receiving therapeutic foods and formula through the ward kitchen. This model, now active in several African countries, represents a scalable, low-cost solution to address hospital malnutrition in resource-limited settings.
References
1. Makamo N, Schoon S, Ozuah N, Kaspers G, Ladas EJ, Huibers M. Prevalence of undernutrition in children with cancer in low-income and middle-income countries: a systematic review. BMJ Glob Health. 2025;10(6):e019345. doi:10.1136/bmjgh-2025-019345
2. Brinksma A, Sanderman R, Roodbol PF, et al. Malnutrition is associated with worse health-related quality of life in children with cancer. Support Care Cancer. 2015;23(10):3043-3052. doi:10.1007/s00520-015-2674-0
3. Orgel E, Sposto R, Malvar J, et al. Impact on Survival and Toxicity by Duration of Weight Extremes During Treatment for Pediatric Acute Lymphoblastic Leukemia: A Report From the Children’s Oncology Group. J Clin Oncol. 2014;32(13):1331-1337. doi:10.1200/JCO.2013.52.6962
4. Orgel E, Genkinger JM, Aggarwal D, Sung L, Nieder M, Ladas EJ. Association of body mass index and survival in pediatric leukemia: a meta-analysis. Am J Clin Nutr. 2016;103(3):808-817. doi:10.3945/ajcn.115.124586
5. Abdulrhman MA, Hamed AA, Mohamed SA, Hassanen NAA. Effect of honey on febrile neutropenia in children with acute lymphoblastic leukemia: A randomized crossover open-labeled study. Complement Ther Med. 2016;25:98-103. doi:10.1016/j.ctim.2016.01.009
6. Ladas EJ, Blonquist TM, Puligandla M, et al. Protective Effects of Dietary Intake of Antioxidants and Treatment-Related Toxicity in Childhood Leukemia: A Report From the DALLT Cohort. J Clin Oncol Off J Am Soc Clin Oncol. 2020;38(19):2151-2159. doi:10.1200/JCO.19.02555
7. Al Jaouni SK, Al Muhayawi MS, Hussein A, et al. Effects of Honey on Oral Mucositis among Pediatric Cancer Patients Undergoing Chemo/Radiotherapy Treatment at King Abdulaziz University Hospital in Jeddah, Kingdom of Saudi Arabia. Evid-Based Complement Altern Med ECAM. 2017;2017:5861024. doi:10.1155/2017/5861024
8. Clark LF. Are innovative ready to use therapeutic foods more effective, accessible and cost-efficient than conventional formulations? A review. Outlook Agric. 2020;49(4):267-277. doi:10.1177/0030727020932184
9. Salam RA, Das JK, Bhutta ZA. Integrating nutrition into health systems: What the evidence advocates. Matern Child Nutr. 2019;15 Suppl 1(Suppl 1):e12738. doi:10.1111/mcn.12738
10. Bazzano AN, Potts KS, Bazzano LA, Mason JB. The Life Course Implications of Ready to Use Therapeutic Food for Children in Low-Income Countries. Int J Environ Res Public Health. 2017;14(4):403. doi:10.3390/ijerph14040403
